Large, heavy breasts can contribute to a range of physical symptoms, including discomfort, restricted movement, and challenges with posture or physical activity. These concerns may affect day-to-day activities such as clothing choice, exercise, or sleep. For some individuals, these challenges may begin in adolescence and continue into adulthood.
Breast Reduction surgery (Reduction Mammoplasty) is a procedure that may be considered to address physical symptoms associated with breast size. Dr Gary Kode, Specialist Plastic & Reconstructive Surgeon based in Melbourne, offers consultations to discuss whether this procedure may be suitable. He performs all surgeries himself, providing continuity of care from initial consultation through to post-operative review.
Why people consider Breast Reduction (Reduction Mammoplasty) Surgery
There are many reasons individuals may consider undergoing Breast Reduction surgery and while each patient is unique some reoccurring reasons include:
- Chronic musculoskeletal pain: Ongoing pain in the upper back, shoulders or neck caused by the weight of the breasts pulling forward on the spine and soft tissues. This can lead to poor posture and contribute to long-term strain on joints and muscles.
- Skin irritation or infection: Moisture and friction under the breast fold can lead to persistent rashes, yeast infections, or skin breakdown, particularly in warmer weather or after exercise.
- Grooves or indentations from bra straps: Heavy breasts can cause bra straps to dig into the shoulders, leaving red marks, pain, and even nerve compression in more severe cases.
- Difficulty with physical activity: Many women find certain exercises, especially high-impact or cardiovascular activities difficult or uncomfortable. This can limit overall fitness and mobility.
- Challenges with clothing: Finding supportive bras or professional clothing can be frustrating. Some patients also report unwanted attention or feel their breast size is out of proportion with the rest of their body.
Men with gynecomastia, or enlarged male breast tissue, may also be candidates for reduction surgery.
Am I a Suitable Candidate for Breast Reduction (Reduction Mammoplasty)?
Breast Reduction surgery may be considered by individuals who experience physical symptoms or functional limitations related to breast size, like those mentioned above. Other factors that may indicate suitability include:
- Being in good general health, with no medical conditions that could affect healing or surgical outcomes.
- Being a non-smoker, or willing to stop smoking well before and after surgery.
- Understanding the risks, potential complications, and limitations of surgery.
- Having completed childbearing, as pregnancy and breastfeeding can affect the outcome.
- Being at or close to a stable weight that has been maintained for at least six months.
- A commitment to maintaining a balanced lifestyle, as significant weight fluctuations after surgery may impact results.
During your consultation, Dr Gary Kode will carefully assess your health history, goals, and physical condition to determine whether Breast Reduction is an appropriate option.
Types of Breast Reduction (Reduction Mammoplasty) Techniques
The technique used for your Breast Reduction depends on a number of factors, including the amount of volume to be removed, your skin quality, degree of breast ptosis, and desired outcome. Each technique involves different incision patterns and scar placements.
Dr Gary Kode customises each operation and typically uses one of the following techniques:
1. Wise-Pattern (Anchor) Technique
The anchor incision (also known as the Wise pattern or inverted-T incision) typically used in cases involving significant excess skin and tissue. This approach allows for comprehensive reshaping and repositioning of the breast. The technique involves three incisions:
- Around the areola – to allow for repositioning and, if necessary, resizing of the areola.
- Vertically from the bottom of the areola to the breast crease – enabling removal of excess skin and access to underlying tissue.
- Horizontally along the inframammary fold (breast crease) – to assist with reshaping and achieving a desirable size.
Once the incisions are made, excess breast tissue, fat, and skin are removed. The remaining tissue is reshaped into a more proportionate size. The nipple-areola complex is typically moved to a higher position on the chest wall, maintaining its connection to underlying nerves and blood supply when possible. The areola may also be reduced in diameter for increased balance.
This technique provides significant control over breast shape and skin removal, making it suitable for individuals with considerable breast volume, skin laxity, or asymmetry. While the anchor incision does result in more visible scarring compared to other methods, scars generally fade over time and are typically positioned so they can be concealed under clothing and undergarments.
2. Vertical (Lollipop) Technique
The vertical/lollipop technique, is typically used when individuals are seeking a moderate reduction in breast size with reduced scarring compared to traditional methods.
This technique involves two key incisions:
- Around the areola – to facilitate repositioning and, if required, resizing of the areola.
- Vertically from the bottom of the areola to the inframammary fold (breast crease) – allowing for removal of excess tissue and skin, and enabling reshaping of the breast.
Unlike the anchor incision method, the vertical technique does not involve a horizontal incision along the breast crease. This reduces the overall length of the scar while still permitting a significant reshaping of the breast mound and elevation of the nipple-areola complex.
During the procedure, excess glandular tissue, fat and skin are carefully removed and the remaining breast tissue is reshaped. The nipple-areola complex is typically repositioned to a more central, elevated position while preserving its vascular and nerve supply.
Final results depend on individual anatomy, healing characteristics, and the extent of tissue removal required.
3. Peri-areolar (Donut) Technique
The peri-areolar breast reduction, also referred to as the donut or Benelli technique, is a breast reduction approach involving a single circular incision around the edge of the areola. This method allows for:
- Removal of excess skin in a concentric ring around the areola.
- Repositioning of the nipple-areola complex, when necessary.
- Mild to moderate reshaping and lifting of the breast.
During the procedure, a ring of skin is excised around the areola. The surrounding tissue is then tightened and sutured to the outer edge of the areola, effectively reducing the skin envelope and allowing for repositioning. Because the incision is confined to the areolar border, scarring is typically limited to this area, which may fade over time and is often camouflaged by the colour transition between the areola and breast skin.
This technique may be suitable for individuals seeking a moderate reduction in breast volume with limited skin excess or for those requiring nipple-areola complex repositioning without significant reshaping of the breast tissue.
While the peri-areolar technique is less invasive than vertical or anchor methods, it does have limitations. It may not be suitable for individuals requiring removal of a larger amount of breast tissue or those with significant breast ptosis (descent of breast tissue).
Choosing a Breast Reduction (Reduction Mammoplasty) Technique
The selection of a suitable Breast Reduction technique is based on a detailed clinical evaluation and consultation with a Specialist Plastic Surgeon such as Dr Gary Kode. The approach is tailored to each individual, taking into account factors such as breast size, skin quality, degree of tissue descent, nipple position, and personal goals.
Dr Kode applies techniques that prioritise preservation of nipple-areola complex sensation and blood supply while aiming to achieve a balanced, proportional breast shape. The chosen method is carefully matched to the individual’s anatomical characteristics to support optimal surgical outcomes.
Surgery for Breast Reduction
Breast Reduction is performed under general anaesthetic in a fully accredited hospital. In Melbourne, Dr Gary Kode operates at Ramsay Surgical Centre Glenferrie and Masada Private Hospital, both of which provide experienced staff and post-operative care facilities. The following steps are typically involved:
- Pre-operative markings: While the patient is standing, Dr Gary Kode marks the breasts to plan the agreed incision pattern and guide tissue removal, taking into account breast position and proportions.
- Anaesthesia: A qualified anaesthetist administers general anaesthesia. Local anaesthetic is also used in the surgical area to assist with post-operative discomfort.
- Tissue removal and reshaping: The chosen surgical technique (discussed and agreed upon prior to surgery) is used to remove excess skin, glandular tissue, and fat. The remaining tissue is reshaped and repositioned to change proportions and breast position.
- Nipple repositioning: In most cases, the nipple-areola complex is repositioned to a higher point on the breast while maintaining its blood and nerve supply. For patients requiring a significant volume reduction, a free nipple graft may be necessary.
- Drains: Small surgical drains may be placed temporarily to assist with fluid removal and support the early healing process. These are typically removed within a few days.
- Support garment: A post-surgical compression bra is fitted at the end of the procedure to assist with swelling and support the breast throughout the healing period.
Most patients remain in hospital overnight and are reviewed by Dr Gary Kode the following day. Ongoing follow-up care is provided to support recovery and monitor outcomes.
Breast Reduction Before & After Photos
A dedicated gallery of before-and-after photos is available during consultation to help patients visualise outcomes. These clinical photographs, shared only with full written consent, highlight the variety of surgical goals, body types, and results achieved. More photos can be seen during a consultation.
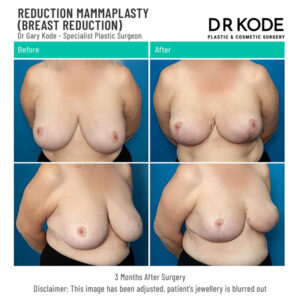

Viewing real cases helps set realistic expectations and provides insight into what can be achieved under Dr Gary Kode’s care. The gallery includes examples of:
- Large volume reductions with significant reshaping
- Moderate reductions with increased symmetry and lift
- Alleviation of asymmetry or nipple malposition
Disclaimer: Individual results vary depending on factors such as age, skin quality, medical history, and overall health. All surgical procedures involve risks. Photographs are not intended to guarantee outcomes.
Recovery After Breast Reduction (Reduction Mammoplasty)
Recovery following Breast Reduction surgery is a gradual process that will vary between individuals. Factors such as your general health, the extent of the procedure and the specific technique used all influence healing time. Dr Gary Kode provides clear post-operative guidance tailored to your needs and remains involved throughout the recovery journey.
Early Recovery (First 1–2 Weeks)
- Mild to moderate swelling, bruising, and discomfort are to be expected in the early days and are typically managed with oral pain relief.
- Drains (if used), are usually removed within the first 1–2 days.
- A post-surgical bra or compression garment is worn continuously to help reduce swelling and support the breasts during the early stages of healing.
- It is important to rest with the upper body slightly elevated, avoid lifting or stretching and begin with slow walks to support circulation.
Ongoing Recovery (Weeks 3–6)
- Most patients feel more comfortable by this stage and may resume light daily activities or return to desk-based work.
- Swelling gradually subsides and external dressings may be removed or replaced with scar-supportive tape depending on Dr Kode’s advice.
- Physical activity remains limited, particularly any exercise that involves the upper body.
- Follow-up appointments allow Dr Kode to monitor healing and address any concerns.
Later Recovery (After 6 Weeks)
- Many patients are able to return to full activities, including travel, exercise and more active work duties, between weeks 6 and 8. This will depend on individual recovery and medical clearance.
- Scars continue to mature and may soften and lighten in appearance over several months.
- It’s recommended to continue wearing supportive bras and to protect healing skin from sun exposure.
Throughout your recovery, Dr Gary Kode and his team remain available to provide advice, reassurance and clinical care to support you during your recovery.
Potential Benefits of Breast Reduction (Reduction Mammoplasty)
Every person is unique, and the potential benefits of surgery will vary depending on individual circumstances, body proportions, medical history, and personal goals. While outcomes differ from one patient to another, potential benefits may include:
- Relief from physical discomfort – including back, neck, and shoulder pain that may be associated with larger breast volume.
- Support for postural alignment – the redistribution of weight may assist with more balanced posture.
- Ease of movement – some individuals find it more comfortable to engage in physical activities or exercise.
- Reduced skin irritation – the procedure may help address issues such as chafing, sweating, or rashes under the breast fold.
- Proportional appearance – the breasts may be brought into alignment with overall body proportions.
- Less strain from bra straps – heaviness in the breasts can contribute to grooving or discomfort from bra straps.
- Adjustment of size differences – in cases of noticeable asymmetry, breast reduction surgery can help increase symmetry.
About Breast Reduction (Reduction Mammoplasty) Scars
Scarring is an expected part of any surgical procedure, including breast reduction (reduction mammoplasty). The appearance, location, and visibility of scars will depend on several factors, such as the surgical technique used, individual healing characteristics, skin type, and adherence to post-operative care instructions.
Immediately after surgery, scars may appear raised, red, or firm. With time, most scars tend to soften and fade. This process can take several months to a year or longer. Regular follow-up appointments allow Dr Kode to monitor healing and guide your scar care routine, which may include the use of silicone tape, topical treatments, or scar massage.
While scars are permanent, their visibility often reduces over time. Their final appearance depends on several individual factors, including genetics, skin tone, and commitment to scar management strategies such as sun protection and non-smoking.
If you have a history of thick or raised (hypertrophic or keloid) scarring, be sure to discuss this during your consultation so that it can be factored into your surgical planning.
Cost of Breast Reduction (Reduction Mammoplasty) Surgery
Surgical fees can vary depending on several factors, including:
- The complexity and duration of the procedure
- The hospital chosen for the surgery
- The type of anaesthetic and who administers it
- Whether drains, garments, and follow-up visits are included
Some patients may be eligible for Medicare or private health rebates if their Breast Reduction is “medically necessary”. In this case, an item number may apply.
As per AHPRA guidelines, exact fees cannot be published online. A comprehensive quote will be provided during your consultation with Dr Gary Kode in Melbourne, based on your needs and any eligibility for rebates.
Risks of Breast Reduction (Reduction Mammoplasty) Surgery
All surgery carries risks. Risk and potential complications of Breast Reduction include;
- Infection or wound healing issues: Particularly in larger reductions or patients with certain medical conditions.
- Changes in nipple sensation: Some patients experience temporary numbness or, in rare cases, permanent loss of sensation.
- Asymmetry: Differences in size, shape, or nipple position may occur and may require revision.
- Bleeding or haematoma: Rare but can require intervention.
- Poor scarring: Some patients may develop thick, raised or pigmented scars, particularly if prone to keloid formation.
- Inability to breastfeed: While most techniques preserve breast function, breastfeeding ability may be reduced.
Dr Gary Kode takes every precaution to reduce risks, including pre-operative assessment, careful surgical technique, and comprehensive post-operative monitoring.
For more information please visit our risks and complications page.
FAQs About Breast Reduction (Reduction Mammoplasty) Surgery
Considering Breast Reduction (Reduction Mammoplasty) in Melbourne?
Book a Consultation with Dr Gary Kode
If you’re considering Breast Reduction surgery or would like more information about your options, we invite you to get in touch. Dr Gary Kode offers comprehensive consultations to assess your needs, discuss potential outcomes, and answer any questions you may have.
To book a consultation or speak with our team, please contact us. We’re here to support you with clear, tailored advice every step of the way.


